
Founded in 2011, Okyanos (pronounced “Oh – key – AH – nos”) is an innovative stem cell therapy provider that specializes in treating patients with congestive heart failure (CHF) and other chronic conditions. The literary name Okyanos, the Greek God of the river Okyanos, symbolizes the restoration of blood flow. Okyanos Cell Therapy delivers a mixed population of fat (adipose) derived stem and regenerative cells (ADRCs) using internationally-approved technology to patients with chronic, degenerative conditions. Okyanos is fully licensed under the Bahamas Stem Cell Therapy and Research Act and adheres to U.S. surgical center standards.
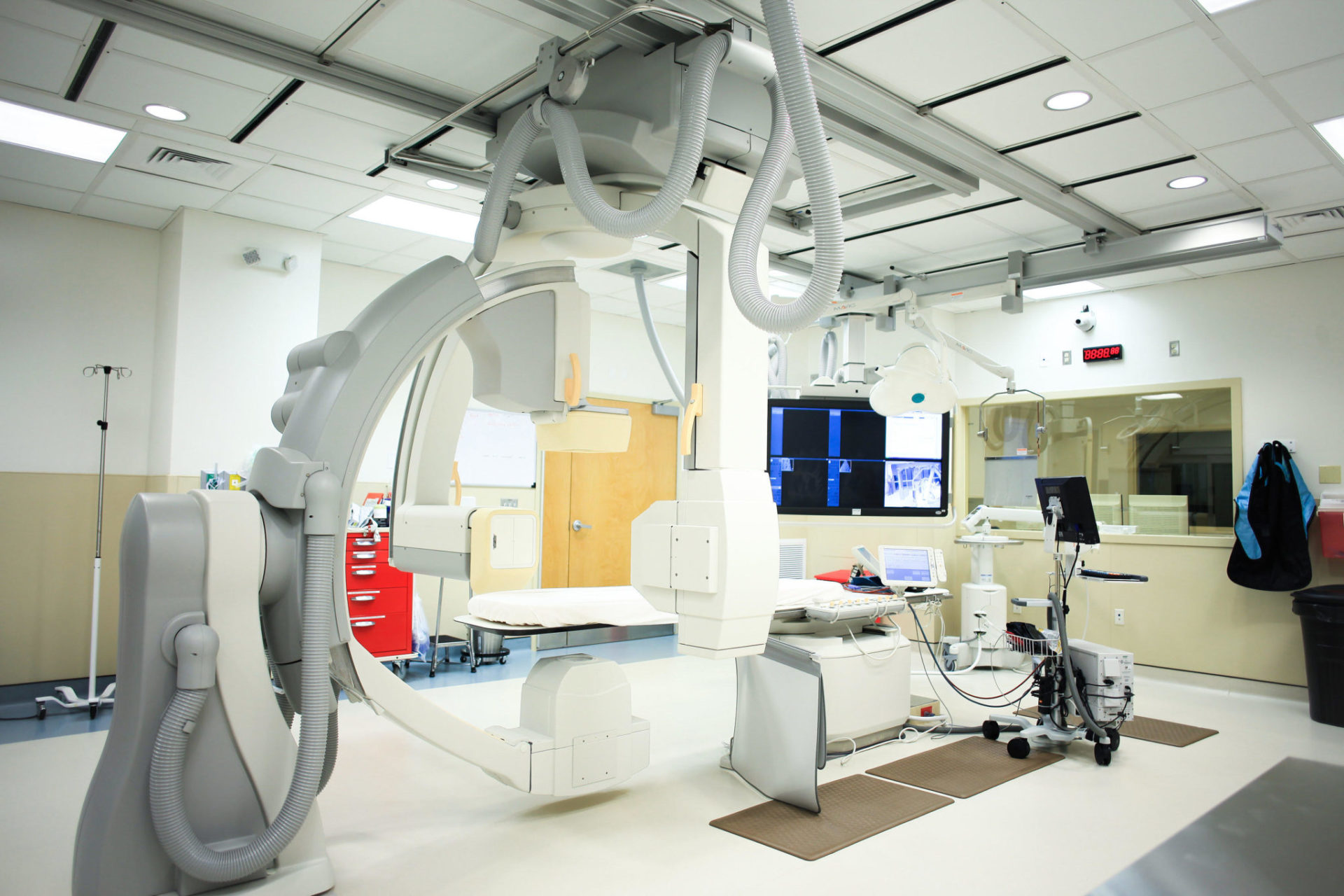
 Okyanos’ stem cell treatments are performed in its purpose-built, state-of-the art cell therapy center, led by Dr. Jeffrey Hartog, a U.S. double board-certified plastic and cranio-maxillo facial surgeon. Treatment is available to patients with severe congestive heart failure, (CHF), osteoarthritis, neuropathy and other chronic, degenerative conditions.
Okyanos’ stem cell treatments are performed in its purpose-built, state-of-the art cell therapy center, led by Dr. Jeffrey Hartog, a U.S. double board-certified plastic and cranio-maxillo facial surgeon. Treatment is available to patients with severe congestive heart failure, (CHF), osteoarthritis, neuropathy and other chronic, degenerative conditions.
While Matthew Feshbach’s career as an investor spanned more than 30 years, he changed directions in 2009 when he and his brother, Joseph Feshbach, began researching the potential of adult stem cells. Their interest resulted from a chance meeting with the public company, Cytori Therapeutics, having been introduced by an investment associate. Extensive research led Mr. Feshbach to believe that stem cell therapy could provide an answer to the largest unmet healthcare need in the Western world, cardiovascular disease as well as many other indications with related disease factors.
Enjoy this interview with Okyanos CEO and Co-Founder, Matthew Feshbach. It is part one of a two-part interview.
Interview with Matt Feshbach, Co-Founder of Okyanos
Cade Hildreth: What is your background and how did you get involved with Okyanos?
Matthew Feshbach: I have a 30-year background as an investor in public companies and was known for doing very deep research on a relatively limited number of potential investments. An investment friend had told me about “personalized medicine” and stem cell therapy and suggested that Cytori Therapeutics had technology that was perhaps more advanced and ready for clinical applications than other stem cell therapy companies. I became very intrigued and then called researchers, from Israel to Japan and Los Angeles to New York, to learn more.
After extensive research I had the realization that cell therapy would be the next phase in the evolution of medicine and it could be as big, if not bigger than the personal computer was to computing and the Internet was to information, or what social media platforms have been to communication.
Cade Hildreth: How was Okyanos founded and who provided the initial investment?
Matthew Feshbach: Myself, my twin brother Joe, and my partner, Manuel Vianna conceived the idea and collaborated in founding Okyanos. Unfortunately, my twin brother passed away of a heart attack about 12 days after we received funding.
Okyanos has been funded by a group of what I would call “purpose-driven entrepreneurial investors.” They are not typical angel investors, because they do not do a lot of these kinds of deals.They nevertheless saw an opportunity to create something meaningful in healthcare, and they believed they would get a high return on their investment.
Cade Hildreth: What was the process of building out Okyanos’ facilities and the team?
Matthew Feshbach: To give you a little background, adult stem cell therapy is not approved in the United States unless it is anything other than within the FDA’s definition of “minimally manipulated,” and this includes stem cell therapy with adipose tissue (fat). Bone marrow does not have the attention of the FDA, but stem cells from fat clearly do have their attention.
On the other hand, Cytori had adult stem cell technology that was approved in Europe and is now approved in Asia (Japan, China, Singapore) and Australia. However, it is not approved in the United States, so I saw an opportunity to bring it somewhere near-shore to a legitimate country, and that was The Bahamas.
We started in The Bahamas, and it took several years because we helped them draft legitimate, rational, and serious regulation and legislation that will keep the stem cell charlatans out of the country.
It was a 3-year process of gaining government approval, building out the facility, selecting our medical team, and treating our first patient. It was not easy, but compared to the United States—where an approval for a drug on average costs about 2.5 billion and take 15 years—I would say that 3 years is pretty good.
Cade Hildreth: How did you attract your medical team?
Matthew Feshbach: Our medical team came about through personal relationships and they all have one common denominator: they see that adult stem cell therapy as the next phase in the evolution of medicine. Also, we have invested more in doing adult stem cell therapy the “right way” than anyone in the world. No one has invested as heavily in technology, the facilities, team and protocols, as we have, and continue to do. We hear from visitors from all over the world say, “Wow, I can’t believe this place.”
Our team has evolved, and we have built an outstanding group.
Our Director of Clinical Operations and Cell Therapy Surgeon is double-board certified plastic and Cranio-Maxillofacial Surgeon, Dr. Jeffrey Hartog. He had been involved with cell therapy since 2010 and has worked regularly with the Cytori technology, so he was interested in becoming more involved.
We also have Dr. Matthew Mick, an interventional cardiologist who is triple board certified (FACC, FACP, FSCAI) and trained at Cleveland Clinic. He was also intrigued with cell therapy. He was a bit of a skeptic when we met him, which is good. We would rather have some who is a healthy skeptic rather than a wild-eyed pioneer. He found that the technology really worked and now he is a huge believer in a cardiac cell therapy, especially after seeing the results.
Our Chief Medical Officer is Dr. Eric Duckers. He was one of the pioneers in cardiac cell therapy in Europe and started with the first trials in 2001. He is the principal investigator of the ADVANCE clinical trial, which treats patients within 24 hours of an acute heart attack using cells from adipose-derived stem and regenerative cells (ADRCs). He had also served as an investigator for the PRECISE clinical trial, which treated patients with CHF , after they had exhausted all options from conventional treatment, and upon which the Okyanos cardiac cell therapy protocol is based.
Our patient educational consultant is Dr. Moira Dolan, board-certified in internal medicine. Dr. Dolan, as an internist, has a thorough knowledge of chronic degenerative disease and which conditions could potentially benefit from ADRCs.
Cade Hildreth: What is the core technology on which Okyanos treatments are based and what type of stem cells are utilized?
Matthew Feshbach: We use cells derived from fat. The generic term for that is stromal vascular fraction, or SVF. The stroma is the connective tissue in the fat and in there are blood vessels. The fraction of cells that come out of that, the inner lining of those blood vessels, are the stromal vascular fraction. We do not use the term SVF, because we know we have a higher quality product, both in terms of safety, yield, and potential efficacy. We call these cells Adipose-derived Stem and Regenerative Cells, or “ADRCs.”
Because we use Cytori’s technology, these cells are a well-documented cellular product. We know what is in the population of cells that we are delivering back to that patient.
The Cytori device also has a CE mark with both therapeutic and safety claims and Japanese approval as a Class 3 medical device. Also, they have a second enzyme that makes them safe to put in the vasculature.
Cade Hildreth: Why did you choose the Bahamas and how is it is an optimal environment for Okyanos?
Matthew Feshbach: We put Okyanos in the Bahamas for three reasons. First, the location is near the US shore. Freeport is only a 22 minute flight from Miami and is within an hour-and a-half to two hours for over half of the population of the United States. It is very convenient.
Second, The Bahamas are a tightly legislated jurisdiction with robust regulations.
Third, the government of the Bahamas wants to be a leading venue for cell therapy, but is committed to only licensing doctors and providers who are doing it at a very high standard.
To be clear, there are a lot of stem cell providers who call me and say, “Hey, we would like to come in to do cell therapy using your facility.” The Bahamian regulators will not allow that, because they want companies who are serious and will make investments in technology, infrastructure and regulatory approvals.
Their regulations require us to have substantial evidence for both safety and efficacy. To date, there have been over 65,000 papers written on mesenchymal cells. There have been over 30,000 papers written on endothelial progenitor cells. There been over 5,000 on adipose-derived stem cells. Meaning, the scientific literature supporting what we do is broad and deep.
Cade Hildreth: What types of patients does Okyanos treat?
Matthew Feshbach: That question is best answered by first looking at the pathophysiology associated with most chronic, degenerative diseases.
First, there is inflammation. Second, there is an immune response. Third, a lack of blood flow (ischemia) or vascular dysfunction. Fourth, there is scarring and tissue degeneration. Our cells, whether they go into the heart or into the blood stream or the joint, have mechanisms that address those factors.
For example, I was reading a paper today on how important endothelial progenitor cells (EPCs) are to autoimmune diseases, because of the micro-vascular dysfunction involved with autoimmune diseases.
Okyanos has broad approvals to treat multiple chronic degenerative diseases,but we do not treat conditions where there is no evidence. Obviously, some things have more evidence than others, and we let our patients know that too.
What we have really come to specialize in is being able to treat a patient for multiple conditions (co-morbidities) in a single setting, when that patient had no real prior relief even after seeing multiple specialists. This is truly a new paradigm in medicine.
The key thing is to understand that the cells are multipotent, which has been documented in tens of thousands of papers. Professor Arnold Caplan, who is fondly called the Father of MSCs [mesenchymal stem cells], put it well by likening these cells to “drug stores” for sites of injury or inflammation.
These cells can work on more than two things at a time and that’s just pretty extraordinary.
Cade Hildreth: What types of improvements have you observed in these patients?
Matthew Feshbach: Our orthopedics program has been outstanding and we have treated more than 200 joints including hips, shoulders, back, knees, and ankles. We have done also very well with rheumatoid arthritis and psoriatic arthritis. To the best of my knowledge, we only have one patient who received our orthopedic protocol and later opted for surgery.
We have done well with certain neurodegenerative conditions as well. With these conditions, because they can progress very rapidly, it can be difficult to get a potent enough dose. One thing that we uniquely understand is that dose matters. By just getting a few cells into an affected area, you might see some moderate but generally unsustainable benefits. However, if you get a robust number of cells into the patient that are highly viable and are true, nucleated cells, then the results can be pretty stunning both in terms of degree and sustainability of improvement. We are beginning to hear reports of our cardiac patients improving from baseline past a year out. That has surprised and delighted them as well as us.
Stem cells work. The key is that when you have people with chronic, degenerative diseases who are in their 50s, 60s, or 70s, which is a large percentage of our patient demographic, you have to get to get them a very potent dose.
The trouble is that by the time you get to age 80, the number of stem cells in your bone marrow goes from 1 in every 10,000 cells to 1 in every 2 million cells.
Adipose stem cells are not affected by age in the way that bone marrow cells are. We can basically take a mixed population of cells and say, “Good, we’re going to bring in reinforcements where they are needed, and there are going to be a lot of them, not just a few.”
Click here to read Part 2 of this Q&A interview with Matthew Feshbach.
About BioInformant
BioInformant is the first and only market research firm to specialize in the stem cell industry. BioInformant research has been cited by major news outlets that include the Wall Street Journal, Nature Biotechnology, Xconomy, and Vogue Magazine. Serving industry leaders that include GE Healthcare, Pfizer, and Goldman Sachs, BioInformant is your global leader in stem cell industry data.





















Stem cell research is the key to developing cures for degenerative conditions like Parkinson’s and motor neuron disease.
La investigación de células madre es la clave para el desarrollo de curas para enfermedades degenerativas como el Parkinson y la enfermedad de la neurona motora.